 By Dr. Laura A Hanyok
By Dr. Laura A Hanyok
Assistant Dean, Johns Hopkins Graduate Medical Education Office
Imagine being a new intern at Johns Hopkins. You have graduated from an international medical school and are eager to start your career as a physician by pursuing leading-edge graduate medical training in the United States. You are aware of the stresses of residency and are mindful of the need to prioritize your well-being during your years of training. Fortunately, you know that Johns Hopkins has taken a progressive approach to promoting clinician well-being in their training program. Over the next year you see these initiatives in action.
On orientation day, you hear a presentation from the leaders of the Graduate Medical Education (GME) office. They frankly discuss the challenges in residency training, including stressors you might encounter and the increased suicide risk that residents have compared to young adults who are not physicians. This helps to normalize your concerns. They also share information about the resources that the hospital and university provide, and ask you to think about what your support system will be while you are in training. As an international medical graduate, this piece particularly resonates with you, as you realize you may not have the same established support system as other colleagues who have more friends and family nearby.
Before orientation, you were invited to an optional training in resilience skills. This is designed to help you be more resilient, and to be equipped to provide “emotional first aid” to your colleagues. You weren’t able to attend this training but hear from some other interns that it provided them good tools to use.
As your first week begins, you receive an email sent to all residents and fellows called “Wellness Matters.” The GME office sends this to you weekly. There are different topics each week – they may remind you to establish care with a primary care physician on campus, use your free gym membership, or notify you about events happening on campus and within Baltimore that support your well-being. They also include a link each week to an article to read that helps you to reflect on the meaning you find in your work as a physician. This gets you thinking about your well-being even when you are very busy on your rotations.
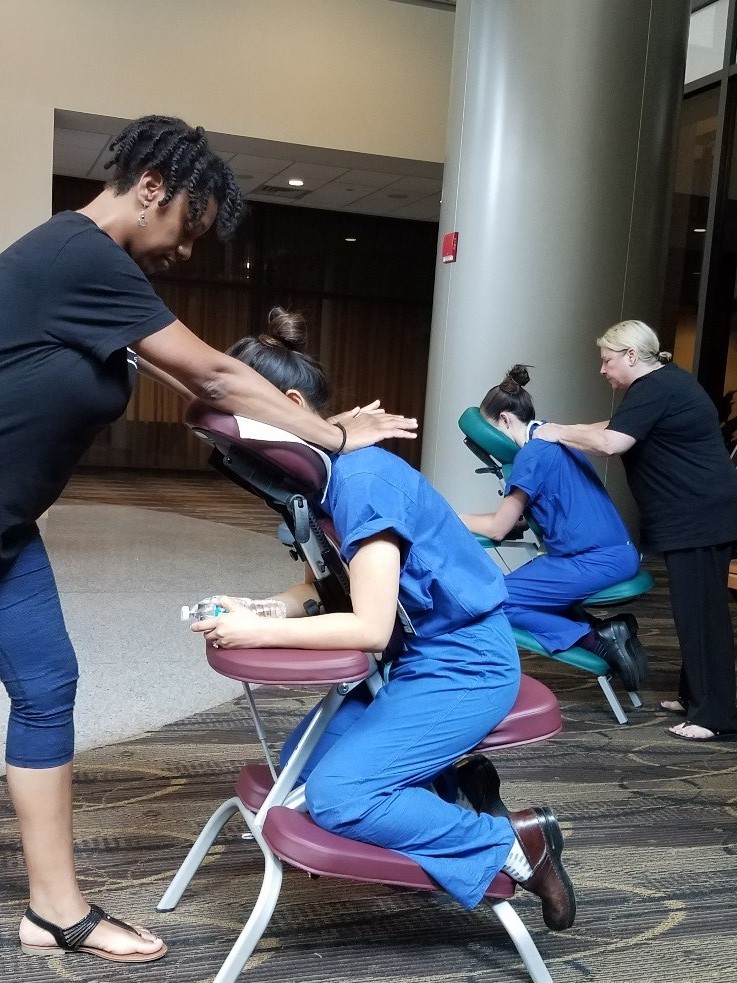
Occasionally you make it to Wellness Wednesday. This is a weekly event that gives residents a chance to relax and take care of themselves. You stop by for free yogurt and other snacks, a seated massage, and time to sit with your colleagues. On a less intense rotation, you make it to a late afternoon yoga session that is free for residents. A colleague of yours who is a parent attends a dinner workshop about self-care for residents who are parents.
Sometimes you make use of hospital and university resources to help your well-being. After a long shift where you feel unsafe to drive, you take an Uber home that your program reimburses you for. You call the RISE program to get “emotional first aid” after one of your patients unexpectedly dies. You look to the wellness webpage created by the GME office (wellness.som.jhu.edu) to find out how to schedule a mental health appointment. On the webpage you also find some useful resources to help with mindfulness.
Over the holiday season you aren’t able to get home. You are thankful that the hospital has celebrations for Christmas and New Year’s that you can take part in. Some nurses even invited you to their homes over the holidays. You really appreciate this thoughtfulness.
In the winter, your Housestaff Council (that represents and advocates for all residents) holds Resident Appreciation Week. This has been happening for several years, and was the spark that would grow into the larger well-being programming that the GME office now organizes. Different events happen during appreciation week – there is breakfast with hospital leadership, a Friday happy hour, and visits from pet therapy dogs.

As spring arrives, you decide that you want to become more involved in what the hospital is doing to support residents. When you start your PGY-2 year, you become a representative on the Housestaff Council, and learn that the council has a yearly wellness survey that is carefully reviewed by the GME office. The Associate Dean or Assistant Dean for GME attend your council meeting every month to hear resident concerns.
Although residency continues to be challenging and sometimes difficult, you feel supported both by your program and by the GME office, and you can tell that residency leaders value you and see your well-being as an important part of your professionalism.
************
Clinician well-being is more than just a trending topic in the medical community. Data shows that clinician burnout can impact the quality of patient care and have serious consequences for the clinician, ranging from poor job satisfaction to depression, and even suicide.
Johns Hopkins School of Medicine has invested in these well-being programs to support our residents and fellows in both their day-to-day training and in the whole of their graduate medical education. In this way, we promote happy, healthy residents and happy, healthy patients.
